'Making the right choices in ITP management and care' – A shared decision-making toolkit for patients.
To download click this link:
Making the right choices in ITP management and care
Groundbreaking new toolkit launched to support patients with rare blood condition to take ownership of their care
- Shared decision-making toolkit developed for people with Immune Thrombocytopenia (ITP) - a rare autoimmune blood disorder that causes a shortage of platelets and bruising.
- Toolkit developed via a multi-stakeholder ITP Expert Working Group led by the ITP Support Association and the UK ITP Clinical Forum.
- The toolkit will facilitate improved treatment and care by empowering and educating patients – and reminding healthcare professionals – about the importance of ongoing collaborative decision making in the management of ITP.
As part of Global ITP Awareness Week (20-25 September), the ITP Support Association and the UK ITP Forum are pleased to launch Making the right choices in ITP management and care – A shared decision-making toolkit for patients.
The toolkit is a response to the results of a patient survey made by the ITP Support Association in 2020. The survey highlighted inconsistencies in the diagnosis and management of ITP – which can negatively impact patients.
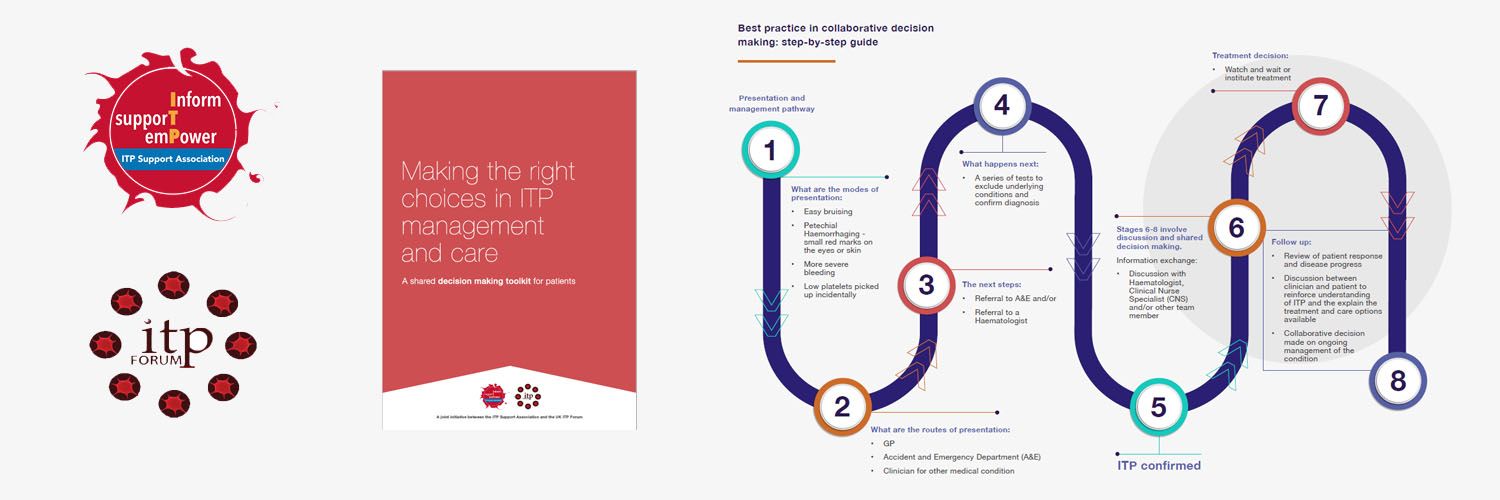
It defines what best practice collaborative decision making in ITP management and care looks like and provides a practical guide to help patients, carers and healthcare professionals achieve this.
This material allows the patient to develop knowledge, skills, and the confidence needed to make managed and informed decisions about personalised health and care. It will ensure that more ITP patients are on care plans that appropriately suit their lifestyle and individual circumstances, improving their quality of life – which can be severely impacted if an individual is placed on a suboptimal care plan.
This toolkit is groundbreaking in that it is one of the first haematological conditions to develop specific guidance in response to National Institute for Health and Care Excellence (NICE) recommendations for shared decision-making practices to be implemented across all conditions.
The toolkit is endorsed by the Royal College of Pathologists and Genetic Alliance UK and the ITP Expert Working Group and partners are calling for this best practice guidance to be adopted across all healthcare settings in the UK.
Professor Adrian Newland, Chair of the ITP Support Association, said:
“Following our recent patient survey, the ITP Support Association identified significant disparities between patient experiences of care and whether individual preferences were considered in care management plans. We decided that we should bring together a group of haematologists with a particular expertise in ITP to develop this toolkit that, we hope, will empower patients to hold collaborative and honest discussions with their clinician which in turn will result in better outcomes and quality of life.”
Dr Quentin Hill, Chair of the UK ITP Forum, said:
“The ITP toolkit is an excellent introduction and companion document to support and empower patients. It guides them step by step though the journey of diagnosis and medical care. A collaborative approach is more rewarding for patients and clinicians, and I have no hesitation in recommending that the ITP Toolkit is given to all patients at presentation.”
Dr Sue Pavord, Consultant Haematologist, Oxford University Hospitals and ITP Expert Working Group member said:
"It has been a real pleasure working with patients and the ITP Support Association in preparing this Toolkit. Mutual understanding and joint decision-making is crucial when planning management which is suitable and acceptable to the individual patient. I encourage all NHS trusts and haematological teams to review the Toolkit and refer to the guidance when deciding on treatment and care with an ITP patient.”
The ITP Support Association and members of the ITP Working Group are available for interview and to provide further comment.
Contact: This email address is being protected from spambots. You need JavaScript enabled to view it. 07535 605467
